|
Peripheral constriction, enlarged blind spot and other types of visual field defects (superior, paracentral) were described. In a series, scotoma was described in 61% of cases. Given the circumstances, it is important for the clinician to bear in mind this fact in its diagnostic work-up, given the rarity of npAIR, and to exclude neoplasm.įundus autofluorescence (FAF) can may indicate hyperautofluorescence around the macula and hypoautofluorescence around the optic nerve, hyperautofluorescent ring around the macula and hypoautofluorescent patches in the posterior pole Visual Fields In a series, the most commonly associated finding was hypothyroidism, however, there are other associations described, such as rheumatoid arthritis, multiple sclerosis, autoimmune hepatitis, Hashimoto´s Thyroiditis, myasthenia gravis and graves disease. It is common for patients who have npAIR to have associated systemic pathologies, particularly related to autoimmune dysfunction. 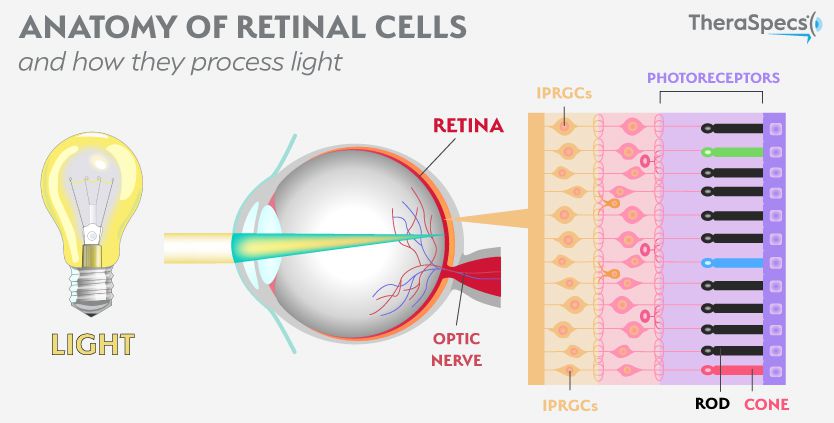
Spontaneous improvement of these symptoms are possible Fundus exam may appear benign, however, some non-specific findings may be present, such as pigmentary changes, retinal vascular attenuation, optic disc pallor, macular edema, retinal atrophy, or retinal pigmentary depositionTypically there is minimal to no intraocular inflammation. Typically patients present with vague and subtle symptoms that are often bilateral and asymmetric including photopsias, dyschromatopsia and nyctalopia. The diagnosis of npAIR is challenging given its rarity, various clinical manifestations, and non-specific findings. Retinal damage of photoreceptors, ganglion cells, and bipolar cells occurs through caspases and intracellular calcium influx apoptotic mechanisms. Ī bacterial or viral infection may trigger the cross reaction of retinal protein and bacterial/viral protein. There have been a number of anti-retinal antibodies found to be associated with npAIR with the most significant being anti-recoverin, anti-carbonic anhydrase II, anti-α-enolase, and anti-rod transducin-α antibodies. Given that the RPE is a major component of the blood-retinal barrier and contributes to immune regulation, it is often the target of the degenerative progress. PathophysiologyĪlthough the mechanism of the disease is not yet fully understood, it is thought to be caused by circulating autoantibodies against the retina causing destruction of photoreceptors and widespread degenerative changes in the retina and retinal pigment epithelium (RPE). npAIR is associated with autoimmune disease, most commonly hypothyroidism. The disease is more prevalent in females (63–66%) and typically occurs between the fifth and sixth decade of life. In 1997, the first case of npAIR was described and its clinical similarity to cancer associate retinopathy (CAR) was noted. but the term “paraneoplastic retinopathy” was used to describe malignancy-associated AIRs by Klingele et al. The first case report of paraneoplastic AIR (specifically, cancer-associated retinopathy) was published in 1976 by Sawyer et al. Given this delay in diagnosis and treatment initiation, the visual prognosis in npAIR is often poor. Variable disease expression is thought to be due to the different permutations of autoantibodies in patients. ĭiagnosis of npAIR is one of exclusion, and is often difficult and delayed given a wide variety of clinical findings and symptoms associated with the disease. It is caused by cross-reactivity of serum autoantibodies to the retina and retinal photoreceptor antigens. NpAIR is characterized by bilateral, rapidly progressive vision loss, visual field defects, and photoreceptor dysfunction. 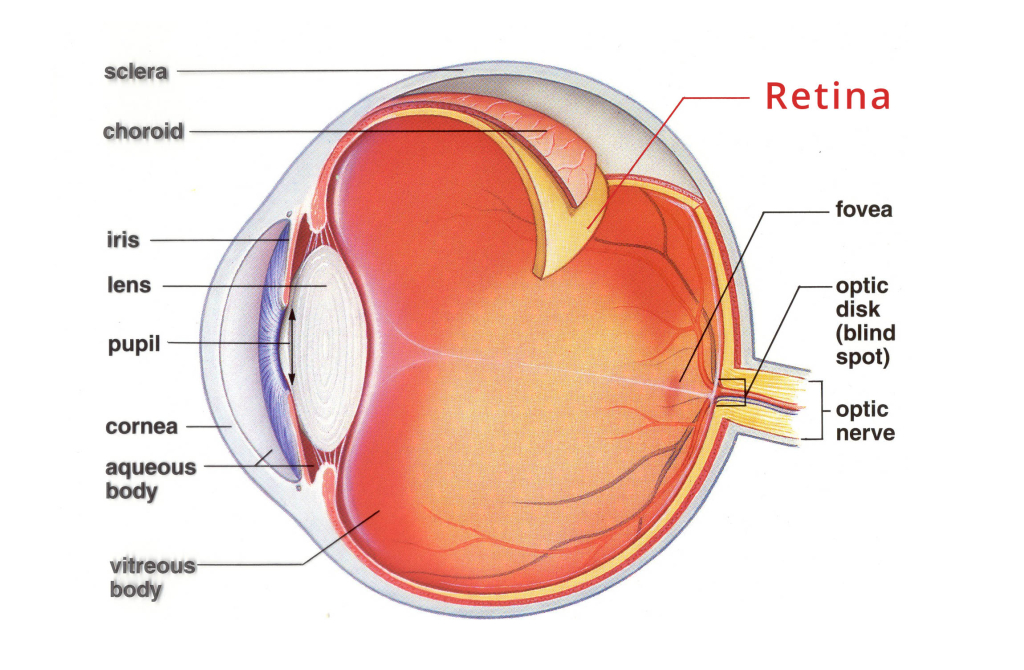
The two main types of autoimmune retinopathy are paraneoplastic retinopathy, which is associated with an underlying malignancy, and non-paraneoplastic autoimmune retinopathy (npAIR) which arises independently of cancer. Autoimmune retinopathies are a rare set of diseases that often lead to retinal degeneration.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
